Got COVID-19? The Answer May Be Right in Front of You
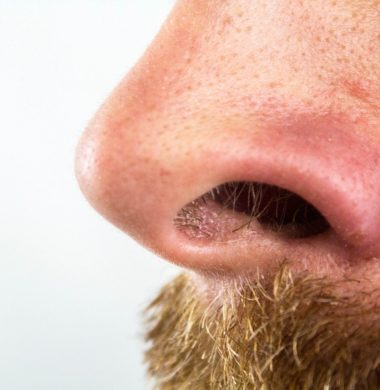
Your nose knows. A sudden loss of smell may indicate that you have been infected by the coronavirus, SARS-CoV-2, the disease known as COVID-19. Testing for smell may be more effective than other tests including temperature checks according to Stoelting Instruments and Scientific Assessments, distributor of the Smell Identification Kit™ (SIT), and Dr. Andrew Badley, physician and researcher in the virus lab at the Mayo Clinic.
A recent publication in the Annals of Internal Medicine, May 2020, looked at smell and taste in 2,013 European patients with mild to moderate COVID-19 symptoms. In younger patients, the presentation of COVID symptoms is quite varied unlike what is commonly reported as fever, cough, shortness of breath, fatigue, and muscle aches. Most patients (87%) reported a loss of smell and 56% of patients reported taste dysfunction. Most patients regained their sense of smell in 5 to 14 days after the smell loss. Rare reports have documented permanent alteration of smell and taste after COVID symptoms.
COVID-19
The theoretical mechanism of the loss of smell lies in how the Coronavirus SARS-CoV-2 enters the body. It is an airborne virus entering the body through the attachment of two receptor sites, ACE2, and TMPRSS2 receptor proteins. These receptors are found in almost every organ system, especially lung, heart, kidney and now realized in the nose. The virus enters these olfactory cells and injures the cilia (hair-like projections that are sensitive to odors and register smell).
Taste and smell are complex functions and taste is often a result of smell, rather than the tongue. The tongue has 5 types of taste buds that are designed to protect us from foods that could be harmful or helpful. The 4 common are bitterness, sour, salt, and sugar. The fifth recently discovered is umami, the “earthy taste” found in mushrooms, soy, and other “earthy” foods.
Smell drives taste and food aroma drives appetite. Eating is a balance of the senses: timing (the clock drives hunger), visualization (sparks anticipation), texture (gives the chew), and taste (the last of the senses in eating). There are several disorders including nasal disorders, allergies, colds, excessive mucous production, MS, and stroke. Loss of smell is often an early sign of Alzheimer’s and Parkinson’s. Age and depression alter smell and taste too.
There are several drugs that can affect taste: certain antibiotics, pain medications, cardiac drugs…digitalis, BP medicines, statins, anti-anxiety medications, chemotherapy drugs, smoking, nicotine, and excessive amounts of zinc.
Some COVID patients have described a total lack of smell (anosmia) or reduced smell (hyposmia). Some have reported that they cannot taste the difference between water or tea. Others have said that everything tastes like metal.
For this reason, eating when you have COVID-19 can be challenging. Adequate nutrition during and after coronavirus is essential. Patients have noted weight loss and muscle wasting with prominent symptoms. In addition, side effects of shortness of breath, coughing, and chest discomfort makes it more difficult to eat.
Here are a few suggestions, remembering that symptoms of COVID can be varied and multiple including sore throat, GI disturbances, etc. Not all recommendations fit everyone:
- It is better to get at least six small meals of snacks each day. Large amounts create more pressure in the abdomen pushing the stomach against the diaphragm making breathing more difficult.
- Hydration is essential, especially with fever. Avoid caffeinated foods. Beverages such as broth, juice, ginger ale for nausea, Jell-O, or popsicles are beneficial.
- Avoid dairy products…milk, etc. These are mucogenic substances. Singers will not consume milk or dairy before any performance. Try substitutes such as almond milk or soy milk.
- Soft foods are great if appetite is not good…applesauce, oatmeal, soups, fruit cups.
- Keep up the protein. When the appetite is low, high protein foods are not too appetizing such as steak, chicken, pork, etc. Chicken broth (Organic Bone Broth by Kettle & Fire) has 10 gm. protein in 1 cup, fat-free and *310 mg sodium, gluten-free as well. Protein shakes, high protein smoothies are great. (*check with your provider if you are on sodium restriction)
- Keep snack foods handy and visual to spark an appetite. Go for some of your favorites, helping you to keep up with the calories…health bars, dried fruits.
If you are diagnosed with COVID-19, be sure to contact your health care provider and carefully follow up at intervals regarding symptoms, progress, and your nutritional status and diet.
We would like to thank Richard Collins, MD (The Cooking Cardiologist) for the content of our blog.
- 9 Tips to Reduce Holiday Stress - December 11, 2025
- 6 Tips for Exercising Outdoors with a Heart Condition - May 19, 2025
- Lifestyle Changes That Can Help Manage Arrhythmia - April 30, 2025
Sign Up
As with any health concerns, your specific treatment program should be discussed thoroughly with your primary care physician as well as any specialists who may need to be consulted – like a cardiologist.
Sign Up

